Rheumatoid Arthritis
Summary
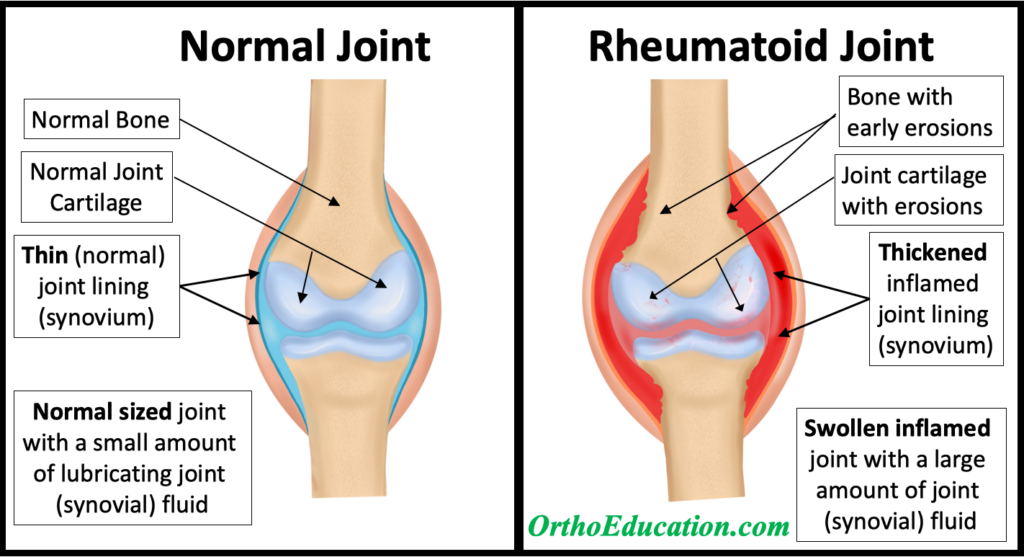
Rheumatoid arthritis is a type of inflammatory arthritis that often causes painful, swollen, and stiff joints. It can affect any joint, but often starts in the hands or feet. In rheumatoid arthritis, the body’s immune system attacks the lining of the joint causing it to become inflamed, swollen, and painful (Figure 1). If not treated early, rheumatoid arthritis can lead to destruction of the affected joints with permanent loss of joint cartilage and long-term arthritis. Early diagnosis and treatment are critical to minimize the long-term damage to the effective joint or joints.
Clinical Presentation of Rheumatoid Arthritis
Patients with rheumatoid arthritis will develop a painful stiff joint or joints with no history of trauma. The condition can occur in any joint, or at any age. However, commonly rheumatoid arthritis begins in the joints of the hand or the foot. It most commonly occurs in individuals age 25 to 45. There is a subset of the condition that occurs in young people known as juvenile rheumatoid arthritis (JRA). Women are more likely to be afflicted with rheumatoid arthritis than men.
Imaging Studies
Rheumatoid arthritis in the early stages will often not demonstrate any specific changes on plain x-rays. However, rheumatoid arthritis that is chronic or poorly controlled will demonstrate x-rays findings that include: loss of bone density, erosion of bone on either side of the joint (peri-articular erosions), and loss of the joint space. The loss of joint space when seen on x-rays demonstrates a loss of the cartilage covering the bones.
An MRI of the affected joint will often show thickening of the synovial joint lining. This MRI finding is not specific to rheumatoid arthritis and may be seen in a variety of other types of inflammatory arthritis.
Bloods Test to Diagnose Rheumatoid Arthritis
A physician treating a patient with a swollen joint or joints may perform a series of blood tests to help determine whether rheumatoid arthritis or another type of inflammatory arthritis may be the cause of the patient’s symptoms. The actual blood tests that are ordered will often be dictated by which condition the physician is assessing for. Common blood tests that may be used to assess for rheumatoid arthritis and other types of inflammatory arthritis include:
- Rheumatoid factor (RF) test
- Anti-nuclear antibody (ANA) test
- Cyclic Citrulinated Peptide (Anti-CCP) antibodies test
- C-reactive protein (CRP)
- Erythrocyte Sedimentation Rate (ESR)
Treatment of Rheumatoid Arthritis
Early diagnosis and treatment is critical in patients with rheumatoid arthritis! Early treatment can often prevent the condition from worsening before irreparable damage to the affected joints has occurred. Fortunately, modern treatment strategies are now much more effective than in previous years.
Effective treatment usually starts with clarifying the diagnosis as there are a number of conditions that can present in a similar manner to rheumatoid arthritis. Referral and assessment by a rheumatologist is often helpful in clarifying the diagnosis and instituting an appropriate treatment plan. Treatment may need to be lifelong in order to prevent irreparable joint damage. There are a variety of medications available that can help treat rheumatoid arthritis. These include:
- Anti-inflammatory medications: Nonsteroidal anti-inflammatory drugs (NSAIDs) such as ibuprofen and indomethacin can be effective in decreasing pain and symptoms. However, NSAIDs do not address the underlying immune-related etiology.
- Disease-modifying anti-rheumatoid drugs (DMARDs): DMARDs provide general suppression of the immune system. They can be very effective and are often used as a first line approach to controlling rheumatoid arthritis. Common DMARDs include methotrexate, sulfasalazine, and hydrochloroquine.
- Biologic medications: Biologic medications such as tumor necrosis factor (TNF) inhibitors target specific components of the immune system. They are more difficult to manufacture, more expensive, and need to be administered via an injection. However, these biologic medications can be very effective at stopping the progression of rheumatoid arthritis.
Surgical Treatment of Rheumatoid Arthritis
At times, it may be beneficial to undergo surgery to help treat a joint afflicted by rheumatoid arthritis. There are two broad categories of surgery that are commonly used: joint preserving and joint sacrificing.
If there is extensive swelling from thickening and inflammation of the joint lining (synovitis) but the joint cartilage is otherwise in acceptable condition, a synovectomy may be beneficial. A synovectomy is a procedure that attempts to remove most or all of the swollen synovial joint lining. It can be done by making an open incision to expose the affected joint, or via an arthroscope placed into the joint.
For joints where rheumatoid arthritis has caused extensive destruction of the joint cartilage more definitive “joint sacrificing” surgery may be necessary. Examples of this type of surgery include:
- Hip replacement surgery for a hip joint that has been extensively damaged by rheumatoid arthritis.
- Knee replacement surgery for a knee joint that has had the joint cartilage irreparably damaged by the rheumatoid arthritis
- Ankle fusion or ankle replacement for definitive treatment of an ankle joint where the rheumatoid arthritis has irreparably destroyed the joint.
- Great toe fusion in patients where the main joint of the great toe (the 1st MTP joint) has lost the cartilage due to rheumatoid arthritis.
July 11th, 2024
